AI Tool Predicts Chemotherapy Benefit in Breast Cancer Using Routine Pathology Slides
A major challenge in the treatment of the most common subtype of breast cancer (Hormone receptor-positive, HER2-negative early breast cancer) is determining which patients truly benefit from chemotherapy. Although genomic tests (such as Oncotype DX®, a 21-gene based assay) have improved decision-making, their high cost, long turnaround times, and limited global accessibility mean that many patients are still overtreated or undertreated. Addressing this unmet need, a group of Technion researchers, led by Dr. Gil Shamai and Prof. Ron Kimmel from the Faculty of Computer Science and Prof Dvir Aran from the Faculty of Biology, together with a large team of clinicians and scientists from the USA, Portugal and Israel, developed a novel artificial intelligence (AI) tool that uses routinely available pathology slides to provide similar clinical insights without requiring specialized genomic testing.
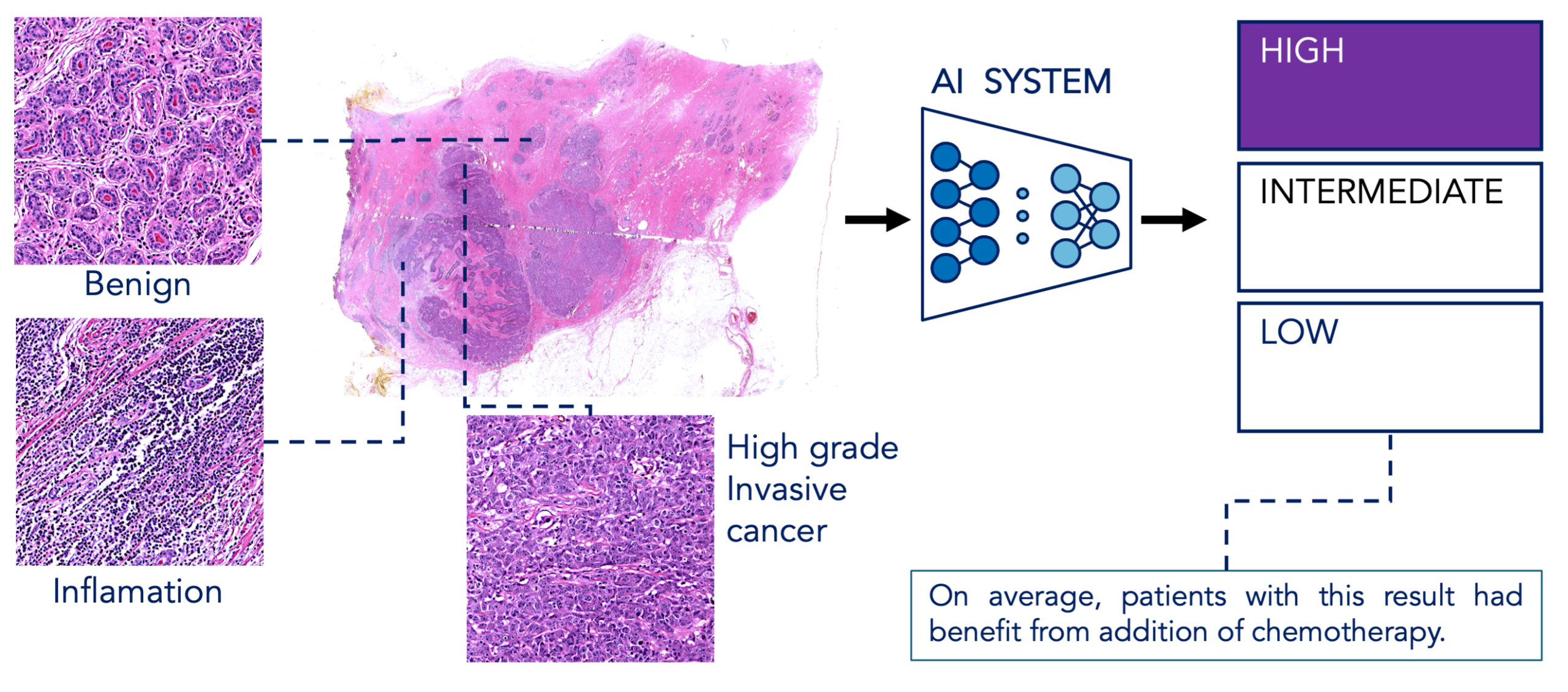
The team created and validated a multimodal deep-learning model that analyses standard pathology slides (hematoxylin and eosin-stained tumor slides) alongside basic clinical data to predict recurrence risk and chemotherapy benefits. Trained and tested using data from the landmark TAILORx randomized clinical trial and validated across more than 5,000 patients in diverse international cohorts, the model demonstrated strong agreement with genomic test-based scores and accurately identified patients who do - or do not - benefit from chemotherapy.
Notably, the approach maintained high performance across different populations, laboratory settings, and disease variants, highlighting its robustness and potential for real-world deployment. By enabling rapid, low-cost risk stratification, the model could support immediate treatment decisions for a substantial proportion of patients.
“This work shows that information routinely captured in standard pathology slides can be harnessed to deliver the same clinically actionable insights as expensive genomic assays,” said Dr. Shamai. “Our goal is not only to complement existing tests where they are available, but to provide a practical and scalable alternative where they are not - helping ensure that more patients receive the right treatment while avoiding unnecessary chemotherapy.” This approach could expand access to precision cancer care worldwide, reduce healthcare costs, and minimize treatment-related toxicity for thousands of patients each year.
The study, published in The Lancet Oncology can be found here.